Science & Health Archives – Marijuana Moment Read More [[{“value”:” A new study finds that people who have used multiple different formulations of psilocybin—including whole mushrooms, mycological extract and a […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” Among U.S. workers, those in the food service and hospitality industries are some of the most common consumers of marijuana, […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” Results of a new yearlong study of prescribed medical marijuana for patients with chronic pain and mental health issues observed […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A newly published review of research on marijuana and chronic nerve pain concludes that treatment with cannabinoids offers “significant relief […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A new scientific review of available evidence on the relationship between cannabis and driving finds that most research “reported no […]
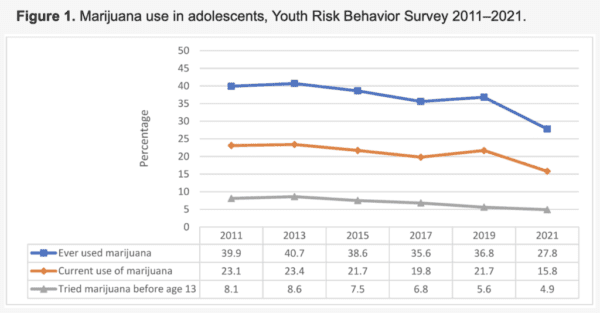
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A newly published study tracks what it calls a “significant decrease” in youth marijuana use from 2011 to 2021—a period […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” There’s “no evidence” to support the idea that there’s a widespread trend of illicit marijuana being laced with fentanyl, a […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A new federally funded study published by the Journal of the American Medial Association (JAMA) analyzed product listings on a […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” Two new federally funded reports published in the Journal of the American Medical Association (JAMA) may help allay at least […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A new scientific review on the insecticidal potential of cannabis concludes that it’s “proved to be a promising plant in […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” A federal health agency is acknowledging that a sizable portion—between about 20 percent and 40 percent—of people being treated for […]
Science & Health Archives – Marijuana Moment Read More [[{“value”:” As many as 6 in 10 people currently receiving treatment for depression in the U.S. could qualify for psilocybin-assisted therapy […]